How Peptide Imbalances Could Be Making You Fat
-
Overweight,
-
Craving carbohydrates,
-
Always feeling hungry and never feeling satisfied after eating,
-
Suffering from immune problems such as asthma, eczema, allergies, or auto-immune diseases,
-
Feeling chronically inflamed with arthritis and body aches and pains,
-
Not sleeping well,
-
Feeling depressed and tired?
You may be one of the millions of people who have high leptin levels.
Most of you know that I don’t like to focus on just one thing when it comes to health problems, but this peptide called Leptin has such a wide-reaching influence and is connected to so many systems that it’s definitely worth looking at to see how it fits in the big picture.
APPETITE
Leptin is probably better known for its role in appetite regulation, and Leptin Resistance (LR), just like Insulin Resistance (IR), is associated with obesity and weight gain.
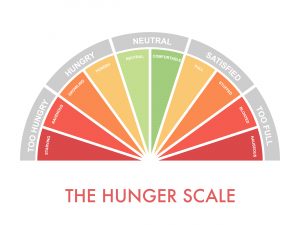 In fact, one of leptin’s major roles is to down-regulate sweet taste receptors on the tongue and thus reducing sweet cravings.
In fact, one of leptin’s major roles is to down-regulate sweet taste receptors on the tongue and thus reducing sweet cravings.
But this is a very one-dimensional model of leptin biochemistry and there’s a lot more to this fascinating peptide. Just like cortisol, leptin oscilates within its own circadian rhythm.
Around 10am – 2pm we experience the lowest levels of leptin. This is when you will experience hunger as low levels of leptin triggers the hypothalamus in the brain to signal the rest of the body that it’s time to eat. So, it makes sense to have your biggest meal at lunch time.
As you consume more calories your leptin levels will progressively rise. Around 12pm or 2am leptin levels will peak, signalling that there is enough fuel on board, so no need to eat more, but certainly time to start burning off some of that fuel.
This is when the mitochondria takes over…
MITOCHONDRIA
These little power houses of the cells will start to burn off the fuel that has been accumulated throughout the day. When leptin is increased in a leptin-sensitive person, mitochondrial function is stimulated and energy breakdown is initiated.
Likewise, if you are Leptin Resistant (LR), low levels of leptin will be the message being communicated between your cells and mitochondrial function (and thus metabolism) will slow down.
This makes it even harder to burn fat and lose weight.
LEPTIN RESISTANCE
This occurs mainly in the hypothalamus. Leptin is initially released from fat cells or adipocytes, then travels to the brain and binds to a leptin receptor (LEPR-B) in the hypothalamus called the arcuate nucleus. By binding to the arcuate nucleus it inhibits NPY (neuropeptide Y) and AgRP (agouti-related peptide) production. NPY and AgRP are two peptides that increases appetite and makes you feel hungry, and since leptin makes you feel less hungry it makes sense that leptin suppresses the production of NPY and AgRP.
Obese people or those with a lot of body fat will produce more leptin than someone with very little body fat. When all of this leptin rushes to the leptin receptor (arcuate nucleus) to let them into the cell, the leptin receptors get so overwhelmed that they then choose to ignore the leptin molecules instead of trying to let them all through.
This is what we call Leptin Resistance (LR).
Because no leptin is being allowed to enter the cell, the message inside the cell is that we need to produce more leptin, even though there are plenty waiting outside. When the body perceives leptin levels to be low, either because you have low body fat, are on a low calorie diet, or you are leptin resistant, it triggers hunger and sweet cravings because you have more NPY, AgRP and ghrelin floating around.
You have to eat more to get more body fat in order to produce more leptin.
This is why obese people still feel hungry and crave carbohydrates, and why they never feel fully satisfied.
Leptin Resistance can occur in response to high triglycerides (as this impairs leptin sensitivity), impaired LEPR-B (leptin receptor) function, or low POMC in the ageing brain.
IMMUNE SUPPRESSION and INFLAMMATION
An interesting observation is that leptin can be both anti-inflammatory and pro-inflammatory.
Too much leptin suppresses the activity of Treg (T regulatory cells) cells which are the key regulatory cells that controls immune function.
Why is this important?
Because Treg cells is the part of our immune system that prevent common problems such as allergies, asthma and eczema. Common health issues found in today’s modern society.
When Treg cells are suppressed, inflammation is left to its own devices with increases in leukotrienes and PGD2 (prostaglandin D2) levels which may be linked to obesity-induced-asthma. This is a key mechanism how body fat and inflammation is linked, and why many ‘diseases’ disappear once we start to lose weight. Rashes disappear, asthma improves, arthritis gets better, etc.
Now when you have a leaky gut you need those Treg cells to come in and clean up the mess. If this is suppressed because of high leptin, then this gut repair cannot happen and the food intolerances, gut dysbiosis and inflammation just get worse.
How many of you struggle to heal your leaky gut?
NEURO-INFLAMMATION and MOOD DISORDERS
It’s a well accepted fact that there is a clear link between the immune system and the brain.
Inflammatory cytokines produced by the immune system in response to infections or other triggers have a direct effect on the nervous system and brain. Cytokines affect neurotransmission (the communication between brain cells), cortisol release and other hormones.
Depression, anxiety, PTSD (Post Traumatic Stress Disorder) and many other mood disorders are now seen as inflammatory disorders of the brain instead of separate diseases.
STRESS RESPONSE and HPA AXIS
Leptin also puts the breaks on CTRH (Corticotropin Releasing Hormone) in the hypothalamus.
CTRH stimulates the adrenals to produce cortisol.
In a nutshell, it means…
If you are Leptin Sensitive or have Lower Leptin secretion, less cortisol or stress hormones will be produced. This means less anxiety and better ability to cope with stress.
If you are Leptin Resistant (LR) or Higher Leptin secretion, you may experience uncontrolled release of cortisol which may give rise to anxiety and contribute to problems with sleep in the long run. Cortisol eventually becomes depleted and we end up with end-stage adrenal fatigue and inflammation that is out of control.
LEPTIN and INSULIN RELEASE
Leptin affects insulin release which is why you often see both Insulin Resistance (IR) and Leptin Resistance (LR) together.
We already talked about how higher levels of leptin and the immune suppression that results from this contribute to higher levels of inflammation. But this also triggers a magnesium loss which can impact on acid/alkaline balance and insulin sensitivity. The result is that less glucose will be transported into the cells, blood sugar levels will increase, and the result of interference in energy production.
The increase in blood glucose levels will trigger more insulin to be released and as you can guess this sets the stage for the subsequent development of Insulin Resistance (IR) for the same reason that you become Leptin Resistant (LR) discussed earlier in the piece.
Metabolic Syndrome and Fatty Liver
A more technical explanation involves TNF-α which is an inflammatory marker produced in higher amounts in fat cells by monocytes/macrophages, usually in response to high leptin in this context. This TNF-α inhibits the activating phosphorylation of the insulin receptor and insulin receptor substrate 1 (IRS1) in muscle and fat tissues.
And this then leads to Insulin Resistance (IR) and reduced insulin signalling.
However, when leptin is balanced it will actually promote insulin sensitivity.
How?
By increasing fatty acid oxidation. Leptin in balance stimulates mitochondrial function and metabolism which will trigger fatty acid oxidation, or the burning of fat as a fuel source. When we burn more fat, we burn more triglycerides which reduces the triglyceride storage in muscle cells.
In fact, leptin has a role in muscle building and is upregulated by exercise and higher protein diets.
LEPTIN and the MICROBIOME
Gram negative bacteria have ‘little tails’ called endotoxins or lipopolysaccharides (LPS). This triggers inflammation and cytokine release, which drives insulin and leptin resistance.
It is one of the big connections between the gut microbiome and metabolic syndrome and how our gut bacteria can make us fat.
SLEEPING HABITS
Loss of sleep or poor sleeping habits can disrupt leptin circadian rhythms.
This is another reason why those who get a good night’s sleep tend to have lower levels of obesity and weight gain, and why shift workers tend to have more problems with maintaining a healthy weight.
ESTROGEN CLEARANCE
Excessive leptin production as seen with leptin resistance may also increase the clearance of estradiol out of the body via upregulation of Cyp1A1 and Cyp1B1 enzymes.
This is because high leptin produces increased amounts of inflammatory cytokines such as TNF-α which makes these enzymes work faster. The problem is that this TNF-α also then downregulates enzymes such as COMT and NQ01 which is needed to further breakdown toxic metabolites of estrogen called quinones which can be very harmful in the body.
This is how you can end up with low levels of healthy estrogen, but higher levels of harmful estrogen metabolites, contributing to symptoms of estrogen dominance without the beneficial protective effects of estrogen.
Essentially, this is what you need for weight loss:
- Low levels of inflammation
- Low TNF-α production
- Higher adiponectin levels
- High adipolin
- Balanced leptin production
- Increased leptin sensitivity
CALORIE RESTRICTION and HORMONE SUPPRESSION
How does restricting calories benefit weight loss?
Well, long term calorie restriction of 1100 calories per day or less cause prolonged suppression of metabolic hormone production including gut hormones for up to a year or longer.
One of the main reasons why gastric bypass surgery leads to weight loss is in fact not to do with the size of the stomach, but the dramatic increase in gut hormones after the surgery. These include incretins such as GLP-1 and CCK which are released when you chew your food properly and aids in weight loss.
This indicates that:
Long term calorie restriction is not the answer for successful weight management.
HCG and PREGNANCY
HCG or Human Chorionic Gonadotropin is a hormone that is secreted in high levels during pregnancy in order to prevent the mother’s immune system from attacking the foetus.
HCG act as an immune modulator which increases Treg cells. It is also used in the popular ‘The HCG Diet’ for weight loss and works in the opposite way to what leptin does. It most likely works through reducing inflammation in the fat cells.
Considering that leptin would be higher in those women who are overweight and those with PCOS (Polycystic Ovarian Syndrome), would it be the suppressive effects on HCG that make these women more vulnerable to miscarriage?
An interesting thought.
At the very least it would have an effect on the neuro-endocrine development of the foetus through epigenetic influences caused by excessive inflammation, interleukin-6 (IL-6) and so forth.
TESTING FOR LEPTIN
Is it necessary to test leptin levels?
Not really.
Testing can be expensive and since leptin can only be secreted by fat cells, body fat composition along with other things can give us a fairly accurate idea of leptin levels.
Generally speaking if body fat percentage is more than 25 for women or more than 20 for men, it is very likely that leptin levels will be in the unhealthy range. This is an important point, because you can get ‘skinny fat’ people.
It is not the size of the person that determines leptin levels, but the percentage of body fat.
Body builders are large but have very little body fat, so they will have very low levels of leptin. Average people with no muscle tone may have very high levels of leptin despite not looking overweight.
LEPTIN IN BALANCE
And it’s always about balance.
You don’t want too much or too little.
It’s not that leptin is bad, but that it needs to be in balance and be able to send the correct signals to keep cells communicating with each other.
EXERCISE and LEPTIN RECEPTORS
Leptin also has a role in muscle building and is upregulated by exercise and higher protein diets.
Leptin promotes insulin sensitivity by increasing fatty acid oxidation and decreasing triglyceride storage in muscle. There are a lot of leptin receptors on muscle tissue cells and exercise improves the function of these receptors and make your body more leptin sensitive. This is just another way exercise suppressed the appetite and improves stress levels. As we increase our muscle mass through exercise and weight training, we improve the ability of leptin and insulin to bind to receptors on the muscle cells, as well as increase the amount of mitochondria available to burn off energy and fat.
What type of exercise is best?
 Fasted Interval Training seems to be the best way to improve leptin receptor sensitivity. This could mean sprinting or walking fast up a hill in the morning before food.
Fasted Interval Training seems to be the best way to improve leptin receptor sensitivity. This could mean sprinting or walking fast up a hill in the morning before food.
Mike Mutzel is a great educator and has done some in depth research into leptin over the years and provides free video seminars that are definitely worthwhile watching if you want to understand all of this better.
Beyond Leptin Resistance: the many ways leptin prevents fat burning
But in the meantime…
WHAT CAN I DO?
- Eat within the time frame of your digestive system’s circadian rhythm.
- Get treatment for any gut dysbiosis you may have that could be interfering with hormone production.
- Exercise in a fasted state.
- Lose weight to increase production of weight loss hormones.
References:
Hormones and bioactive substances that affect peripheral taste sensitivity




Is there a shot of lepton I can take ? Diet excerise not working I gain three – 7 lbs a week please help
Hi Adrihanna, I’m sorry to hear that you’re struggling with your weight.
Taking leptin may not be the answer as you are most likely leptin resistant. Taking more leptin may increase that resistance. The key for you may be to resensitize your leptin receptors. Some compounds like resveratrol and ginsenoside (from ginseng) seem to have properties that can support leptin-sensitising.
https://joe.bioscientifica.com/view/journals/joe/241/3/JOE-18-0606.xml
Other ways to regulate leptin would be to make sure you get enough fibre and polyphenols (compounds in colourful fruits and vegetables) in your diet as these promote gut bacteria and other metabolites that help promote weight loss. Don’t starve yourselve but intermittent fasting may also be helpful.
Make sure you have also eliminated other potential causes for weight gain such as thyroid dysfunction, chronic stress, or hormone fluctuations.