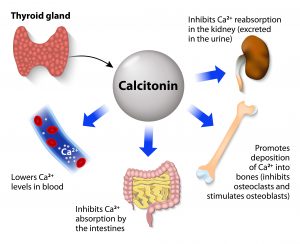
When we think of calcium we generally think of it in terms of healthy bones and teeth. But calcium plays a hugely important role in the body in many other biochemical reactions that have associations with all kinds of chronic and degenerative disorders, via its role in cell signalling and mitochondrial function.
But before we get into that, let’s first discuss the basics around calcium absorption and availability in order to understand why not all forms of calcium are the same.
The Importance Of Calcium in Mitochondrial Function and Regeneration
Calcium is absorbed from your digestive system using an energy-intensive active transport mechanism.
What does this mean?
It means that in order for calcium to go from your gut into your bloodstream your cells have to use quite a bit of energy to make this happen. This is OK if everything is working the way it should, but then, if you are reading this article chances are that you have some kind of chronic health condition that you are trying to find answers for. And this means that your cells are most likely NOT working the way they should, which may impact the absorption of calcium amongst other things.
Most of the calcium you ingest is also absorbed from the small intestine where this active transport mechanism takes place. Many people have gut disorders such as SIBO (Small Intestinal Bacterial Overgrowth) and SIFO (Small Intestinal Fungal Overgrowth) which may impact the functionality of these transporters even further, and possibly have a significant influence on the absorption of calcium.
Then comes in vitamin D.
Those with SIBO/SIFO are likely to have bile insufficiency which could either be a consequence or predisposing factor to their gut issues, or both. We need bile to absorb fat soluble vitamins from our food such as vitamin D. This is something I have lectured on extensively in Australia, New Zealand and the USA.
Bioconcepts Australia and New Zealand 2018 – Mastering the “Great Deceiver”
And what is the role of vitamin D in calcium absorption?
VITAMIN D
 Vitamin D plays a role in the binding of calcium to peptides so that it can be transported to the blood. This is why vitamin D is often recommended along with calcium for enhanced absorption.
Vitamin D plays a role in the binding of calcium to peptides so that it can be transported to the blood. This is why vitamin D is often recommended along with calcium for enhanced absorption.
After vitamin D binds to the nuclear VDR (Vitamin D Receptor), the 1,25-dihydroxyvitamin D3 (active form of vitamin D) upregulates the expression of several calcium transporter genes, such as TRPV5/6, calbindin-D9k, plasma membrane Ca(2+)-ATPase1b, and NCX1. By upregulating these genes transcellular calcium transport is enhanced.
How many people are deficient in vitamin D these days? Plenty from what I’ve seen in my practice. For various reasons such as:
- Living in climates where traditionally there isn’t much sunshine, ie London
- Using sunscreen on a regular basis in hotter climates such as Australia
- Inadequate absorption of vitamin D due to gallbladder dysfunction or insufficient bile production
- Diets low in vitamin D rich foods
- Genetic SNPs on VDR (Vitamin D Receptor) or other related genes
- Inhibition of VDR enzymes due to chronic viruses or other factors
- And the list can go on…
Vitamin D supplementation is also not suitable for everybody, especially those who suffer from chronic infections. That’s a problem when vitamin D is needed to absorb ordinary forms of calcium, because it means calcium deficiency becomes a secondary issue that then potentially worsens cellular communication and mitochondrial function in a population that already has problems in these areas.
So thus far, this is what we need for calcium absorption from most calcium supplements:
- Adequate levels of Vitamin D
- Appropriate genetic expression of important genes such as VDR
- A healthy small intestine, ie no gut dysbiosis
- Enough energy, or good mitochondrial function, to fuel the active transport mechanisms already in place
OK, so again, anyone reading this article most likely has health issues they are dealing with, which means that some or all of these requirements for calcium absorption are likely to be compromised.
The good news is that there is also a vitamin D-independent calcium absorption route where vitamin D is not necessary to get calcium ‘through the gates’ so to speak. This form of passive diffusion becomes very important during certain stages of life such as during the neonatal period, pregnancy and lactation, as well as in those living in climates where sunshine is a luxury.
I’m going to emphasize this point.
IT BECOMES VERY IMPORTANT DURING PREGNANCY, WITH BABIES AND GROWING CHILDREN.
Calcium itself exists in three forms in the body:
- 40 – 45% protein-bound calcium
- 5% inorganic calcium
- 45 – 50% ionized calcium
IONIZED CALCIUM
It is this last form of calcium, ionized calcium, that is the physiologically active form of calcium that is responsible for triggering osteoblast (bone forming cell) and osteoclast (bone dissolving cell) activity by way of regulating thyroid hormone (TH) and parathyroid hormone (PTH) release.
Ionized calcium signals the pituitary gland to secrete parathyroid hormone (PTH) which is the major hormone involved in the regulation of blood calcium levels and allowing for bone remodelling to take place. PTH also initiates the production of 1,25-dihydroxyvitamin D in the kidney via the steroid hormone synthesis pathway.
This means no need for vitamin D supplementation.
But ionized calcium also helps to break the protein-bound calcium in our bodies and cells, and transform them into physiologically active ionized calcium as part of calcium homeostasis. This then allows for these active calcium molecules to function as cell-signalling molecules and regulate calcium homeostasis in return. Essentially taking the calcium that has been storing in areas of your body that it shouldn’t have, and making them more useful.
Calcium can be stored in various tissues and organs where it contributes to many chronic conditions such as:
- Atherosclerosis or hardening of the arteries
- Kidney stones
- Calcification
- Frozen shoulder or other old sports injuries
- Spurs
Yet, despite all of this calcium accumulation, the bones and teeth may be deficient, leading to:
- Osteoporosis or Osteopenia
- Osteoarthritis
- Higher risk of cavity formation in the teeth
IT IS ALL ABOUT QUALITY, NOT QUANTITY
Our bodies also don’t need high amounts of physiologically active ionized calcium. Only small amounts are needed to create the desired biochemical effects that is needed for optimal cell signalling and health metabolism. But because commercial calcium supplements are not in the ionic form, much higher intake amounts are needed to just get a small amount into the cells. When you have too much calcium with nowhere to go, it triggers inflammatory responses in the body and deposits in areas it shouldn’t as previously mentioned.
It is clear that the form of calcium is very important.
More is not always better. It is the form and functionality that is important.
REFERENCES:
https://www.ncbi.nlm.nih.gov/pubmed/25817876
https://courses.lumenlearning.com/suny-ap2/chapter/the-parathyroid-glands/