Sulfur Sensitivities and Why Long Term Avoidance Can Do More Harm Than Good
Many individuals suffering from chronic health conditions have problems tolerating sulfur compounds, whether in food or supplementation. This often becomes problematic as they actively avoid a mineral that is hugely important in helping them get better.
Sulfur occurs in many foods, medications and supplements such as:
- Broccoli
- Onions
- Garlic
- Brussels sprouts
- Cabbage
- Eggs
- Sulfur-based antibiotics such as penicillium
- MSM
- N-acetyl-cysteine
- TMG
Some of the common symptoms associated with sulfur sensitivities include:
But without sulfur the body cannot heal, cannot detoxify, cannot create energy…
The aim should never be to just avoid sulfur, but rather to correct sulfur metabolism and improve tolerance, because look how important sulfur is in the body:
SULFUR AND THE BRAIN
Let’s first look at the role of sulfur in the brain. Once a baby is born, the continual development of brain function and neural connections depend on how available sulfur is to the neurological system.
Sulfur is very important for myelination of nerves and the brain, and also to form perineuronal nets (PNNs) as sulfur is used to form chondroitin sulfate. PNNs occur all around nerve cells where they stabilize the synapses in the adult brain and close critical developmental periods in the child’s brain.
Chondroitin sulfate proteoglycans are needed for brain plasticity, normal ion exchange and GABA signalling between neurons. In fact, PNNs are associated mostly with inhibitory interneurons and balances the excitatory and inhibitory balance in the brain. PNNs preferentially surround GABAergic interneurons and affect GABAa receptors. Heparin sulfate proteoglycans is important for nerve regeneration and synaptic development.
Those familiar with the CBS cycle in methylation will recognize the SUOX and CDO enzymes as part of sulfur metabolism. SUOX and CDO enzymes are the sulfate-synthesizing enzymes that occur on GABA neurons. So, imbalances in sulfur biochemistry will affect GABA production negatively which will have a flow-on effect on moods, anxiety, sleep, progesterone, hormones, and many other functions related to GABA.
GABA is hugely important in regulating autonomic nervous system (ANS) function, healthy digestion and appropriate immune responses. You cannot heal if your ANS is dysfunctional.
But Even Schizophrenia…
“In a series of recently published studies using animals and people, Johns Hopkins Medicine researchers say they have further characterized a set of chemical imbalances in the brains of people with schizophrenia related to the chemical glutamate. And they figured out how to tweak the level using a compound derived from broccoli sprouts.”
Yes, this compound is sulfurophane.
It seems that sulfurophane changes the glutamate imbalances in the brain which may affect how messages are transmitted between the brain cells. Low levels of glutamate is associated with depression and schizophrenia and has been found in lower levels in the anterior cingulate cortex region of the brain in those with psychosis compared to the normal population.
What was even more interesting is that glutathione (further down) seems to act like a storage tank for glutamate. This brings up interesting connections between low levels of glutathione as seen with many toxicity problems and mental health disorders such as Schizophrenia.
You may read more about this in Science News:
Broccoli sprout compound may restore brain chemistry imbalance linked to schizophrenia
SULFUR AND THE GUT
But it’s not just the brain that is dependant on sulfur for healthy function. The digestive system also needs sulfur for various other functions.
For instance, sulfated glycosaminoglycans (GAGs) in the gut is necessary for preventing leaky gut and maintaining nutrient absorption, as well as regulating cholecystokinin and gastrin (intestinal hormones). A study done by Kern et al. (2002) used intravenous porcine secretin in children with autism and found that those with chronic active diarrhea had a reduction in their behavioural symptoms and improvements in language, whereas autistic children with no GI symptoms didn’t show any change. This was interesting as secretin increases the amount of bicarbonate in pancreatic juices and bile. Bicarbonate stimulates sulfate absorption in the ileum of the small intestine via the DRA transporter which is an inflammation-sensitive sulfate transporter that exchanges sulfate for bicarbonate.
So even though I’m personally not a huge fan of using bicarbonates as alkalizers, theoretically, if you took a bicarbonate alkalizer it is possible that you may increase the availability of sulfur molecules and thus GAGs and sulfated mucins, which will improve gut integrity, reduce food reactions, etc.
What does this sound like?
Yes, leaky gut. You need sulfur to prevent or fix leaky gut.
Secretin may also influence sulfate transporters in other locations such as the brain and kidneys, so the aim should be to increase secretin in general.
SO, WHAT IS SECRETIN?
It is a peptide hormone produced in the duodenum of the small intestine encoded by the SCT gene, and is involved in the second part of digestion when the acidic food bolus has moved from the stomach into the small intestine.
Secretin regulates the pH of the small intestine, inhibits gastric acid secretion in the stomach, stimulates bicarb production by the pancreas, stimulates bile production by the liver, stimulates cholecystokin production which makes the gallbladder contract, and increases insulin secretion which prevents blood sugar spikes.
Wow…
…this describes so many of the clients that I see. Because when these functions fail, we end up with gut dysbiosis or organisms growing in environments they shouldn’t be because there’s not enough bile salts to kill them, and the pH creates conditions that favour their growth. And all of this leads to sulfation problems, phenol/salicylate sensitivities, and even oxalate crystal accumulation.
We want to be making sure that we can produce enough secretin to perform all these functions. Secretin is composed of 27 amino acids in a linear structure and has a similar sequence to glucagon, VIP (Vasoactive Intestinal Peptide), and GIP (Gastric Inhibitory Peptide).
We need good protein digestion both for the manufacture of secretin, but also to stimulate its release. When the pH in the duodenum (small intestine) reaches 2 – 4.5 (acidic) or encounters amino acids from protein digestion, secretin is released by cells in the small intestine which triggers bicarbonate release.
HYDROCHLORIC ACID AND SYMPATHETIC INHIBITION
This brings us right back to the stomach and the need for adequate stomach acid to break down protein and create an acidic food bolus.
Remember that the parasympathetic nervous system branch of our autonomic nervous system performs our ‘resting and digesting’ function and needs to be predominant when we eat. If we are constantly stressed or in a sympathetic ‘fight or flight’ response, or deliberately reducing our stomach acid through medications such as antacids or proton pump inhibitors, then we will not produce enough stomach acid and everything we talked about will be slowed or inhibited.
So we’re back to basics where we need to reduce our stress levels, sit down in a relaxed environment to eat, and chew our food properly. Really basic stuff, but so, so important.
But let’s get back to secretin…
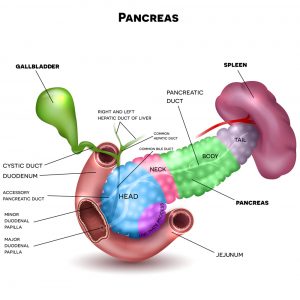
PANCREAS AND ENERGY
Once secretin is released in the small intestine it binds to secretin receptors on the pancreatic cell membranes (centroacinar cells to be more specific). This binding stimulates ATP’s (energy) conversion to cyclic AMP which acts as a second messenger through the purinergic system and triggers the release of bicarbonate. This makes the pancreas a high energy consuming organ that requires functional mitochondria (as this is where energy or ATP is produced).
Those with chronic fatigue or mitochondrial inhibitions from chemicals or toxins will have reduced function, with less bicarbonate being released and less sulfur exchange which will further reduce sulfation and glutathione formation, the very antioxidant so important to keep the mitochondria healthy.
WATER REGULATION
Secretin also modulates water and electrolyte transportation, partly through activating vasopressin release from the hypothalamus which acts in the kidneys to reabsorb more fluid.
So, what potential role could this be playing in bedwetting? Can we associate stress, high cortisol or sympathetic activation, low stomach acid, low secretin, low bicarbonate production, low pancreatic function, mitochondrial dysfunction and poor sulfur exchange with bedwetting in young children?
Interesting thought…
SULFUR AND HEAVY METALS
Sulfate is also very important in the clearance of heavy metals.
The kidneys contain heparan sulfate and chondroitin sulfate proteoglycans which help to bind heavy metals. Once they are bound to sulfate, heavy metals become less-toxic metallo-organic compounds (Ailing et al. 1985). When bacteria is grown in an environment that is deficient of sulfur nutrients, they become more sensitive to mercury and other heavy metals.
Sulfur-hydrogen (-SH) molecules are also known as sulfhydryls or thiols, and are sulfur analogues of alcohol. If you read the article on Phenols and Food Sensitivities you will notice that these are benzene rings with hydroxyl (-OH) groups attached. Thiols have sulfur taking the place of oxygen in the hydroxyl group so -OH becomes -SH. Thiols have a great affinity for mercury (forming mercaptides) and lead which is why these metals can interfere with transsulfuration pathways in the body for which the CBS enzyme acts as the entry-point.
But Also Glutathione…
Glutathione is a major antioxidant protein complex that our bodies make as part of metal and toxin detoxification. Glutathione consists of 3 amino-acids namely cysteine, glycine and glutamate.
Cysteine as explained below is a sulfur-based compound.
And glutamate as explained further above is regulated in part by sulfurophane (another sulfur compound).
CYSTEINE AND THIOLS
When we look at the CBS cycle, homocysteine and serine combine to form cystathionine at the very beginning of this cycle.
The enzyme cystathionine gamma-lyase converts cystathionine into cysteine and alpha-ketobutyrate. The thiol group is the functional group attached to the amino acid cysteine and binds to iron and zinc to form iron-sulfate, zinc fingers and alcohol dehydrogenase. So these thiol groups are very important in the clearance of acetylaldehyde and yeast infections.
But since thiols also have a high affinity for heavy metals we can see how mercury exposure from amalgams for instance can interfere with the functions of iron and zinc in the body. When you have 2 cysteine molecules coming close to each other, it can oxidize where hydrogens are released from the -SH molecules to form a cystine with disulfide bonds (-S-S-), and this is the form most cysteine molecules will find itself in, although free cysteine residues will also be present. Disulfide bonds keep proteins stable and is found in insulin peptides.
When cysteine molecules are exposed to more aggressive oxidants, cysteine gets converted to sulfinic and sulfonic acid.
SO, WHAT’S THE POINT?
Simply to show how important sulfur is in the overall biochemistry and why avoiding sulfur long term may not be the best plan of action if you are reactive to sulfur. This doesn’t mean you should make yourself sick by taking sulfur if you are not processing it well. But it does mean you have to focus on improving your tolerance to sulfur as a long term solution.
But I guess you already knew that 🙂
References:
Wakefield et al. (1998, 2000)
D’Eufemia et al. (1996)
Horvath et al. (1999)
Trends in Autism Research by O. T. Ryaskin
Abnormal Sulfation Chemistry in Autism: Department of Psychiatry, University of Texas Southwestern Medical Center at Dallas – Janet K. Kern, D. Grannemann, Madhukar H. Trivedi; University of Birmingham UK, School of Biosciences and School of Medicine, Division of Medical Sciences – Rosemary H. Waring, David B. Ramsden; Autism Treatment Center, Dallas – Carolyn R. Garver
Broccoli sprout compound may restore brain chemistry imbalance linked to schizophrenia







This is an excellent, well-informed post but it ends on a cliff hanger. How do we improve our tolerance to sulfur as a long term solution?
Hi Liam,
It’s a bit of a million dollar question. If you look at sulfur metabolism there are so many factors involved. Sulfur excretion is regulated by the kidneys, but can also be produced in the gut (as hydrogen sulfide), or poorly converted in the glutathione pathway into PAPS. So for some it may involve correcting gut dysbiosis, for some it may be improving kidney function, for some it may be as simple as adding molybdenum as a cofactor, for some it may be improving bile function for PAPS production. It’s not necessarily a one size fits all.
Thank you for your kind comment 🙂
This is great information and not something I have come across through all of my research! I appreciate the effort put into this! A lot of sulfur intolerance articles and videos are focused around Hydrogen Sulfide SIBO (which may be accurate in some cases) however I think SIBO is simply just another symptom diagnostic tool and not actually getting the the root issue. Do you have any recommendations on how to strengthen the production of secretin?
Hi Linn,
I agree that SIBO is more like a consequence of other factors gone wrong. This is a major reason why so many people suffer from chronic SIBO despite well-designed treatments. Secretin is inhibited by H2 antagonists, such as proton pump inhibitors, which reduces gastric acid. You can support secretin by optimizing histamine which stimulates gastric acid production. But anything that decreases pH will tend to support secretin production such as herbal bitters or betaine chloride supplements. Long-term you do want to focus on healthy vagal nerve function is this is where ANS regulation comes from and thus healthy digestion. The vagus nerve is off course regulated by acetylcholine. That’s another rabbit hole to get into :).